





Welcome
Register
Patient
Multiple Patients
Family Accounts
Insurance Cards
Patient Recalls
Post charges
Electronic Claims
Post Payments
Automatic Resubmit
Aged Reports
In less than two weeks,
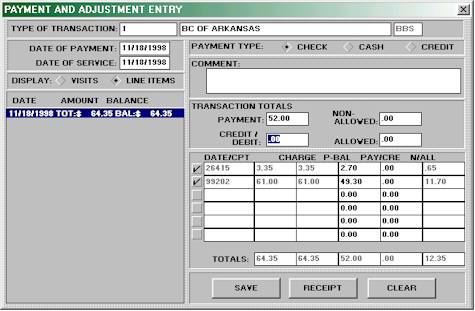
you have received the first payment on a new patients claim. You open
the Information Card, select Payment Entry, and are immediately taken
to the Payment Entry Screen. The payment left a balance of $12.35 which
needs to be billed to a secondary carrier. With the Practice Management
System, this is automatic. In fact, you can setup the software so that
the secondary claim prints as soon as you save the primary payment. Make
a copy of the EOB already in your hands, attach to the claim form, and
your secondary is as good as filed. If the secondary carrier accepts electronic
claims, the secondary is moved to the electronic billing queue.
The system will automatically post your Medicare and Medicaid remittance advice. Instead of manually posting those payments and adjustments, you download the explanation of benefits from the carrier and the ERA module will post the payment and adjustments to each patient's account. This will give your staff more time to work accounts receivable and patient collections.
Home
Contact us
Sales info
Phone - 877.433.4647
Tech support - 800.628.8274
Anesthesia Billing Tour
Medical Billing Tour
Ambulance BIlling Tour